Home > Conditions Treated > Joint Instability/ Ligament laxity
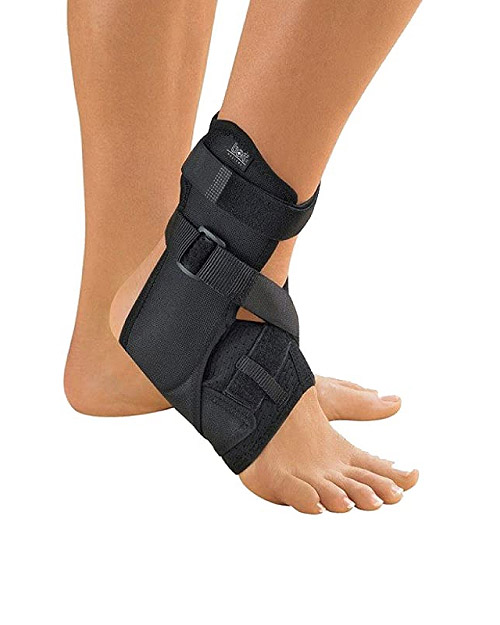
The cartilage within the joint may begin to degenerate when bones become misaligned or when repetitive stress on the joint occurs. Ultimately, the joint may lose all its cartilage leaving it in a state of bone-on-bone without the cushioning effect of the cartilage tissue. At that point the ligaments become overly stretched as they try to support the joint, leading to further ligament laxity and excess motion. The end result is joint instability and disabling chronic musculoskeletal pain.
The human body has 360 joints, each of which contains at least two bones connected to one another by one or more ligaments. The ligaments that connect the bones on each side of the joint may become torn via injury/overuse or otherwise stretched as they try to support the joint, leading to ligament laxity and excess motion in the joint.
The following are risk factors associated with joint instability: History of sprains or dislocations of a joint, engaging in repetitive motions in sports, hobbies, occupations, loose joints, diseases such as Ehlers-Danlos or Marfans, youthful age (i.e. incomplete development of tendons, ligaments, bones). Patients with joint instability or ligament laxity may complain of recurring dislocations or subluxations (i.e. partial dislocations), a feeling of joint looseness or giving out, pain, numbness, or tingling in the joint as a result of injury. Arthritis may an eventual sequela of joint instability as stated above.
Joint instability can be limited or prevented by: minimizing or avoiding high risk and repetitive activities, wearing proper protective equipment during sports, maintaining strength and flexibility in muscles surrounding joints via exercise/yoga/weight training/physical therapy.
Seek care if you experience swelling, bruising, severe pain as a result of physical trauma to the joint or if you have chronic symptoms associated with unstable joints. Medical professionals can usually diagnose a dislocated shoulder by a physical examination and imaging. Plain x-rays can often evaluate the bones of a joint for any displacement or dislocation. Stress x-rays can evaluate the ligament integrity of a joint as well as joint stability.
Non-trauma related instability is treated by strengthening the stabilization muscles around a joint. Physical therapy exercises to improve joint movements and range of motion may also be recommended. Acute trauma-related instability is treated with ice and anti-inflammatory medications. Stabilizing the joint may require temporary use of a sling or brace followed by a physical therapy program of strengthening and coordination exercises.
Regenerative cell treatments such as Prolotherapy, Platelet Rich Plasma or Bone Marrow Aspirate may help heal or otherwise fortify the ligaments that stabilize the joint. Ligaments may become thicker and stronger in the course of this therapy which may reduce the risk of re-injury or dislocation.
Orthobiologic procedures are replacing surgery as an alternative. The aim of using orthobiologic treatments is to support your body’s self-healing processes, reverse disease progression and suppress inflammatory reactions that can worsen pain, leading to symptom relief and recovery of function. We utilize regenerative medicine procedures including patients’ cellular treatments to repair the ligaments naturally.
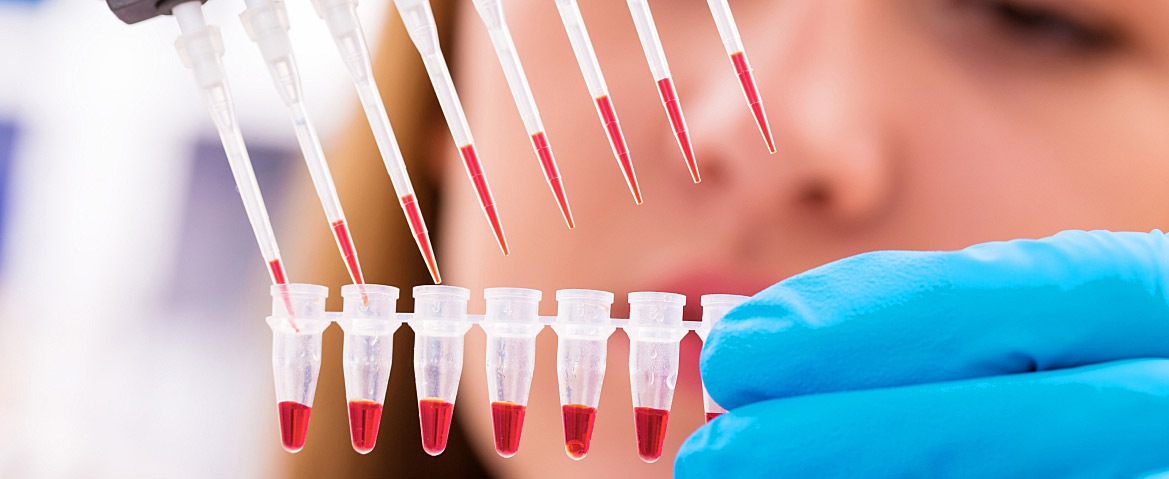
As part of a cell-based treatment, regenerative cells can be collected from bone marrow and blood with minimal discomfort. These cells can then be processed in a state-of-the-art laboratory utilizing the latest technology. Finally, the regenerative cells, in combination with natural growth and healing factors, can be injected where they are needed – such as an inflamed hip or knee joint. Over time, the cells can potentially repair and regenerate the damaged tissues, resulting in relief of pain and improvement in mobility and function.
Surgery to repair and strengthen tendons, ligaments, or muscles is only recommended when
more conservative measures fail.

Although Orthobiologic Cell Therapy is considered by some people to be experimental, various research studies show that some marrow aspirate concentrate and platelet rich plasma injections may provide excellent relief from joint and musculoskeletal pain and ongoing inflammation.