Home > Treatments > Ablation
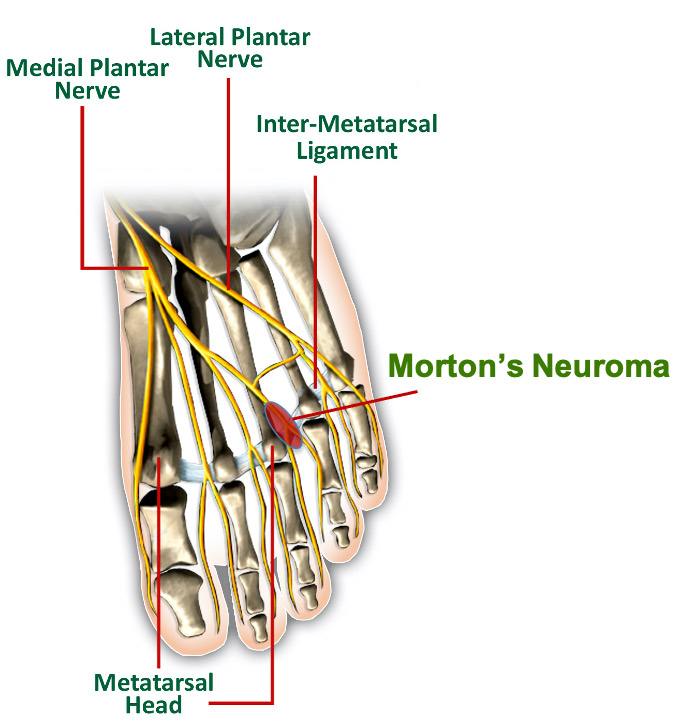
It is common for conservative treatment and corticosteroid injections not to help your Morton’s neuroma or Baxter’s Entrapment. Then, more invasive treatment is warranted. Depending on your other medical conditions and an assessment by our one of our doctors, we perform ultrasound guided ablations. This type of treatment can involve the use of radiofrequency (heat), cryotherapy (cold nitrous oxide), or neurolytic chemicals, (concentrated alcohol.) All our procedures are done under local anesthesia, so they are pain free.
When you come, one of our doctors will do a full clinical assessment of you including a review of your past tests, a full examination of your feet, and an ultrasound guided local anesthetic diagnostic injection. This diagnostic injection is considered the gold standard for the diagnosis of Morton’s neuroma and Baxter’s Entrapment and gives us a good indication as to whether our ablation procedure/s will be successful. Then, we can give you a recommendation as to which of our three ablation procedures is best for you.
Radiofrequency ablation has been used in medicine for many years. Ultrasound guided radiofrequency ablation is a sophisticated, minimally invasive procedure that is associated with high patient satisfaction scores and long-term pain relief. It is a procedure that uses high-frequency radio waves to heat the nerve to 90 degrees Celsius.
At this temperature, the heat breaks down proteins preventing the nerve fibers from transmitting pain. The nerve is destroyed and the pain from that area is not transmitted any further. In addition, radiofrequency ablation may cause the creation of new blood vessels, speeding up the healing process.
Ultrasound guided cryosurgery (also known as cryoablation) is similar to radiofrequency ablation in that it causes carefully targeted injury to destroy nerves to interrupt the pain. It is also associated with high patient satisfaction scores and long-term pain relief.
While radiofrequency ablation uses radio waves to create heat and break down nerves, cryosurgery uses cold/ice instead, using medical-grade nitrous oxide to generate extremely cold temperature to selectively destroy neuroma tissue. It has been used for many years to relieve the pain of various nerve pathologies, including Morton’s neuroma.

Neurolytic injections inject a mixture of a neurolytic agent (usually concentrated alcohol) and local anesthetic directly into the Morton’s neuroma in order to eliminate or significantly diminish the ability of the nerve to transmit pain signals, thereby reducing pain sensation.
It is similar to cyroablation and radiofrequency ablation in that it destroys a small part of the nerve, resulting in pain relief.
It is a mostly painless procedure and you are likely to only feel pain when the local anesthetic is injected into the foot. After the local anesthetic has taken effect, a very small puncture is made over the painful area. The needle is introduced, and an ultrasound is used to guide the positioning of the needle.
In the case of radiofrequency ablation or cryoablation, once the needle is in the correct position, an electrode is placed through the needle and the tip of the electrode is heated (if RF ablation) or cooled (if cyroablation) and repeated according to protocol. For neurolytic ablation, a mixture of the neurolytic agent and local anesthetic is then injected. The site is covered with a bandage and the patient is advised to reduce activity, ice and elevate the foot. The bandage can be removed the following day and the patient can cover the area with a regular Band-Aid. You should keep the injection site clean and dry for at least 24 hours. Reduced activity can be resumed within one or two days of the procedure and any pain that occurs is usually managed with an NSAID or Tylenol. High impact activities on the ball of the foot should be avoided for a week or so. You can drive home on the day of the procedure.
Side effects are not generally seen with this procedure, but a few are a possibility. Infections are rare, as is abscess formation at the puncture site. You may develop bruising that can be painful. Numbness or a lack of feeling in around the incision area can also happen, but this side effect is rare. In the case of cryoablation, frostbite may rarely occur at the area of insertion. You may also feel a small lump in your foot where the procedure was performed. This generally goes away within 3 to 6 months and does not cause pain.
Virtually all Morton’s neuroma patients who have had ablation for Morton’s neuroma have maintained full motor function with no greater loss of sensation then they had prior to the procedure.
You may experience relief from your ablation within a week or 2, but often it takes a longer period of time to heal completely. If there is still pain at eight weeks, the procedure can be performed again.
Most patients find that after 2-3 ultrasound guided ablations their pain has decreased significantly. If, in the very rare case, ultrasound guided radiofrequency ablation has little effect it may be time to look at a different ultrasound guided ablation procedure.
We use ultrasound guidance for all our procedures, and this allows us to visualize the needle tip when administering the treatment, ensuring a higher degree of accuracy. Seeing the needle tip results in a higher degree of success and the prevention of injury to other local tissues. Furthermore, the use of ultrasound can help in the diagnosis of other local pathology, e.g. synovitis, bursitis or tendon pathology. Ultrasound guidance is especially important when using high concentrations of alcohol to ensure that the alcohol sclerosing agent does not leak from the immediate area. If a leak occurs, the neurolytic agent can damage the surrounding structures.